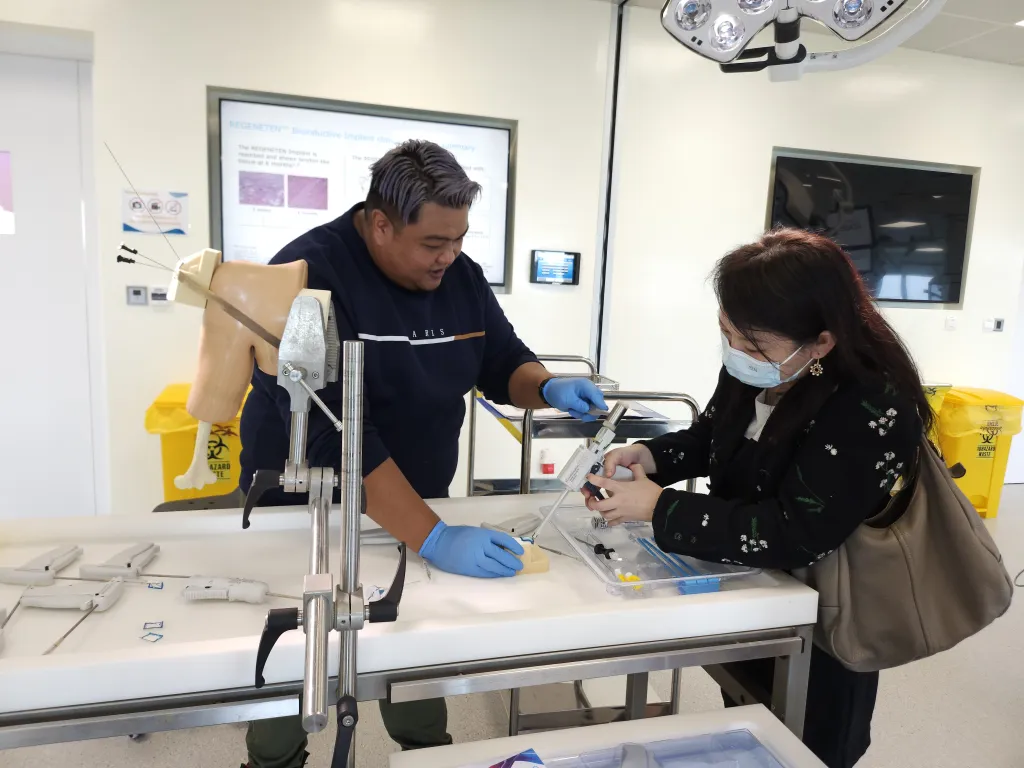
Transforming Hospital Leadership for a Value-Based Future
with SMU Executive Development's Hospital Management Programme

The Challenge
Across healthcare systems in Asia, hospital leaders are confronting a structural tension from traditional healthcare models that are built on a fee-for-service foundation. While effective in expanding access, they prioritise activity over outcomes, leading to unintended consequences such as over-testing, fragmented care delivery, rising costs, and inconsistent patient outcomes.
At the same time, the healthcare landscape is being reshaped by converging structural forces: growing demand driven by ageing populations, chronic disease, and more empowered patient expectations; ongoing supply-side pressures from manpower constraints and operational inefficiencies; and the rapid scaling of transformative health technologies, from AI and telehealth to wearables and genomics.
Yet many hospital systems remain organised around what providers do, rather than what patients need. This creates a fundamental question for healthcare leaders:
How do we redesign healthcare systems to deliver better outcomes that are more efficiently, more equitably, and at scale?
We need to move beyond volume to value; thus the shift toward Value-Based Healthcare (VBHC) popularised by Michael Porter and Elizabeth Teisberg is essential. It demands a rethinking of strategy, financing, operations, and leadership itself.

The Goal
In order to build high-value, patient-centred healthcare systems, senior healthcare leaders set out to address a set of deeply interconnected challenges:
- Driving value and quality simultaneously: Improving clinical outcomes, patient safety, and experience while eliminating waste and unnecessary interventions;
- Designing value-creating strategies: Moving from siloed service lines to integrated, patient-centred care pathways;
- Capturing value through financing and reimbursement: Transitioning from volume-based payments to models such as bundled payments and outcome-based funding;
- Ensuring affordability and accessibility: Building well-resourced systems that deliver high-quality care across all segments of society;
- Leveraging technology meaningfully: Integrating digital health innovations not as add-ons, but as enablers of better care and system-wide efficiency.
Ultimately, the goal was not incremental improvement but a system-level transformation toward sustainable, value-driven healthcare.
The Solution
To address these challenges, Programme Director Dr Markus Karner designed the transformative Hospital Management Programme grounded in the principles of value-based healthcare. Drawing on an integrated curriculum, the programme combines academic rigour with real-world application, equipping healthcare leaders with both conceptual frameworks and practical tools.
Notably, the curriculum incorporated bespoke Asian case studies and real-world insights from healthcare leaders, ensuring relevance to regional contexts. Participants also engaged in interactive discussions, peer learning, and applied problem-solving. The programme’s multi-dimensional learning approach focuses on six critical pillars:

1. Sustainable Healthcare Models: Participants will explore how to design healthcare systems that balance clinical excellence with financial sustainability, using strategic tools to align outcomes with costs.

2. Value-Based Healthcare Strategies: By adopting value-driven outcomes (VDO) frameworks to measure results, we analyse care delivery processes to improve patient experience and outcomes, reduce costs, waste and inefficiencies, and enhance patient journeys across the continuum of care.

3. Operational Excellence: Participants discover the keys to optimising operational efficiency in healthcare by navigating the complexities of healthcare supply chain management to explore resilient-building strategies.
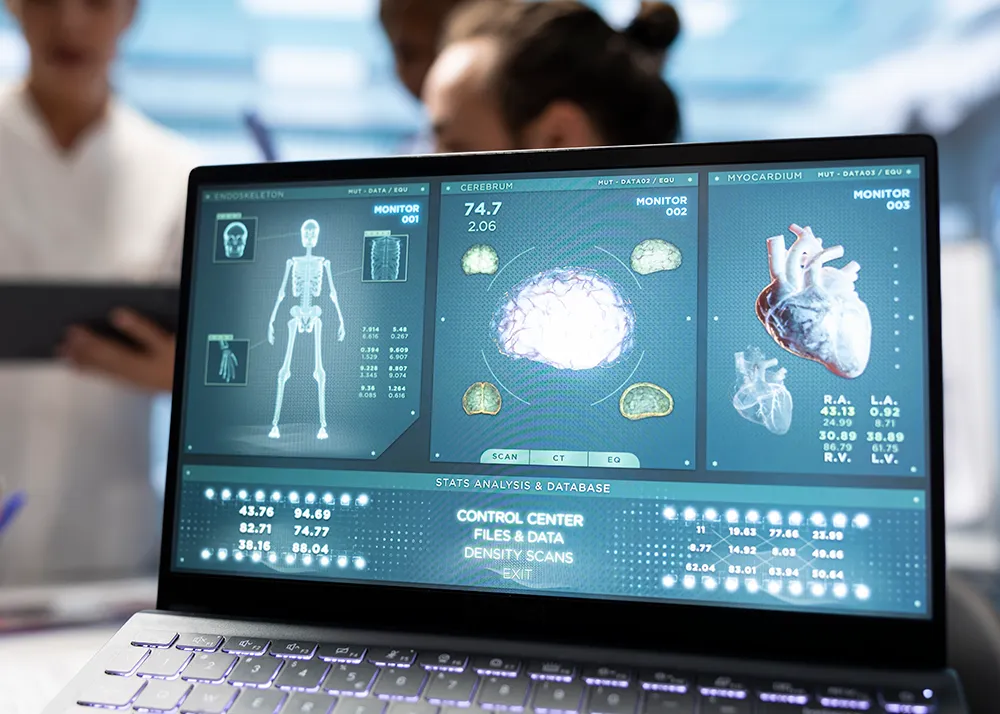
4. Technology and Innovation in Healthcare: The programme addressed the growing role of AI, digital health, and data systems in transforming care delivery, emphasising how technology can enable, rather than complicate, value creation.

5. Community, Wellness and Advocacy: We discuss the topics of community-based interventions and preventive healthcare strategies, aimed at addressing local health needs and to promote healthier lifestyles.

6. Leadership and Systemic Transformations:
Transformation is as much cultural as structural. So, the programme emphasised leadership, mindset shifts, and system-wide thinking, where leaders play a pivotal role in enhancing patient outcomes and optimising healthcare delivery.
The Impact
The true impact of the programme is reflected in how leaders translate learning into meaningful change within systems, teams, and ultimately, patient lives.



The programme fostered a strong network of healthcare leaders across Asia, enabling cross-learning and cross-pollination of ideas between public and private sectors and diverse healthcare systems.
By convening a diverse cohort of healthcare leaders, the programme enabled participants to step outside their institutional and national contexts.
The programme has helped me to widen my horizons to understand more about other health organisations and the healthcare systems in the region. The opportunity to network with both public and private sectors in healthcare is highly valuable.”
—Dr. Asawin Puwatanasan, Assistant Hospital Director, Bangkok Hospital, Thailand
Watch Dr. Asawin's testimonial here.
This exposure accelerated problem-solving by allowing leaders to borrow, adapt, and scale proven ideas across borders, strengthening their ability to design more resilient and future-ready healthcare systems.
Hospital Management Programme
Download Success Story
Check out our gallery >
The ultimate goal of hospital management will always be to align purpose with economic feasibility in a sector that must remain
committed to human values."
— Dr Cheong Wei Yang
Vice Provost (Strategic Research Partnerships)
Singapore Management University,
Senior Adviser (Health Economics),
Ministry of Health, Singapore
Short Courses by SMU ExD
Our programmes provide an opportunity for executives to learn from industry experts, gain insights into emerging trends, and push themselves beyond their comfort zone. with a focus on practical applications and hands-on learning, we offer a unique platform for all levels of executives to develop their leadership skills, advance their careers and widen their professional network.
More information about our Short Courses.
More information about the Hospital Management Programme.